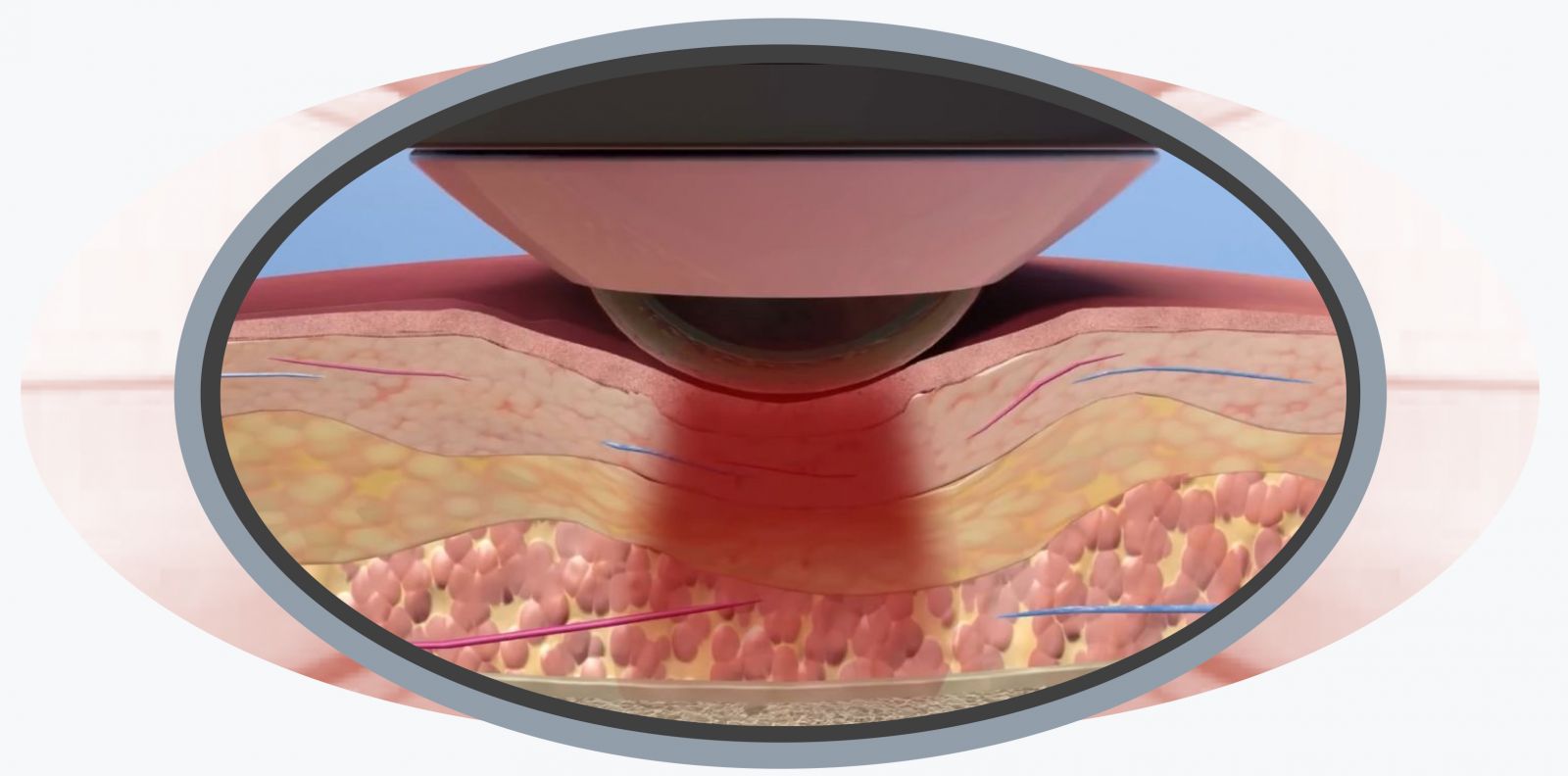
Laser therapy uses a process called photobiomodulation (PBM) This term describes the mechanistic/scientific bases for this photonic specialty. Photobiomodulation therapy (PBMT) is the therapeutic term for its application to change the condition of damaged tissue by stimulating cellular metabolism, thereby accelerating the healing process. As light pours into the tissue photons will be scattered, reflected, and absorbed. Light that penetrates into the tissues can be absorbed by melanin, hemoglobin, oxyhemoglobin, and water. Energy from these absorption events will be dissipated as heat generating a soothing warmth in the tissue. The primary target for photobiomodulation is the cytochrome C complex which is found in the inner membrane of the mitochondria. Cytochrome C is a vital component to the electron transport train that drives cellular metabolism. As light is absorbed cytochrome C is stimulated leading to increased production of ATP the molecule that facilitates energy transfer within the cell. In addition to ATP laser stimulation also produces free nitric oxide and reactive oxygen species.
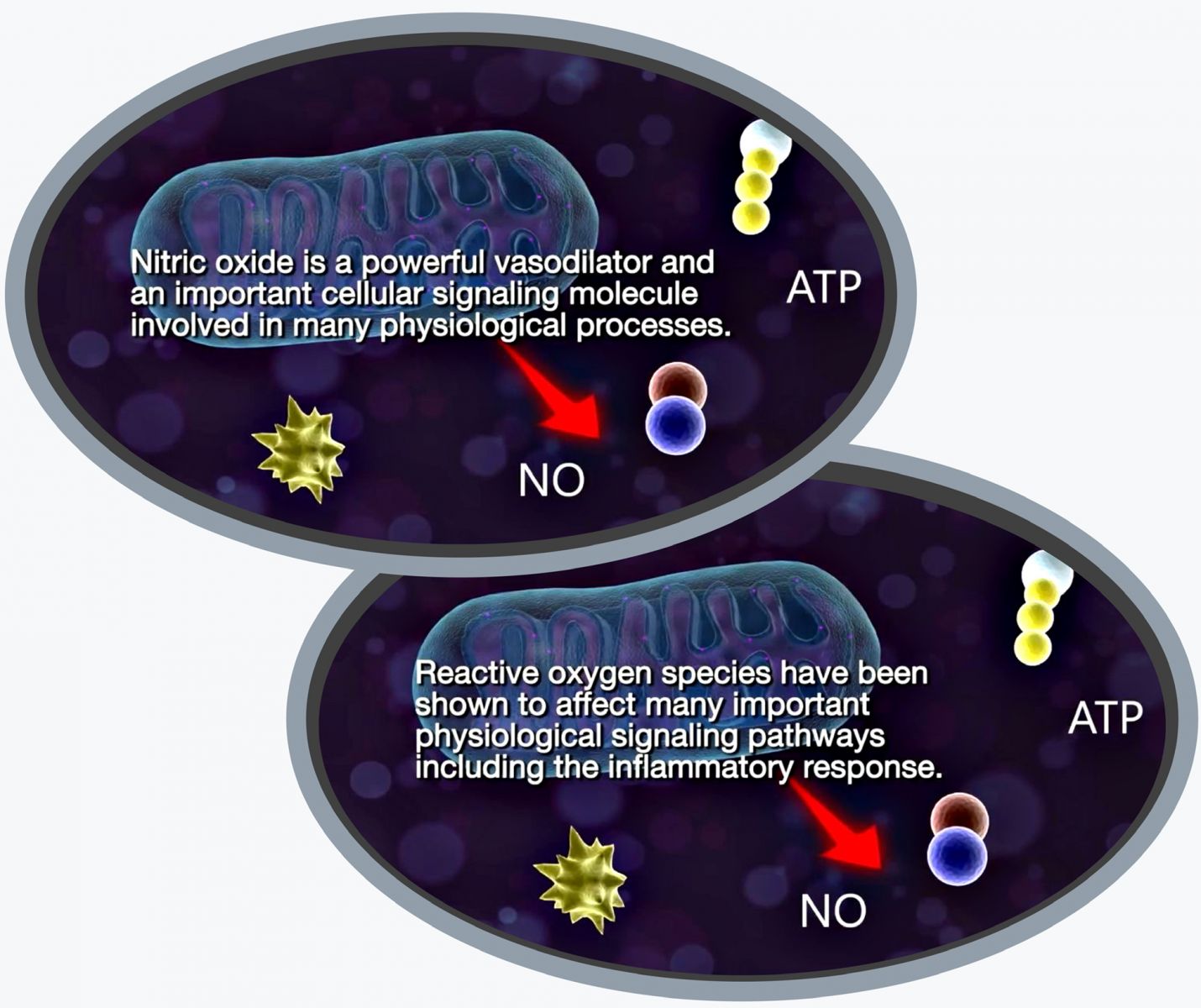
In concert the production of these signaling molecules has been shown to induce growth factor production. To increase cell proliferation and motility and to promote extra cellular matrix deposition and pro-survival pathways.
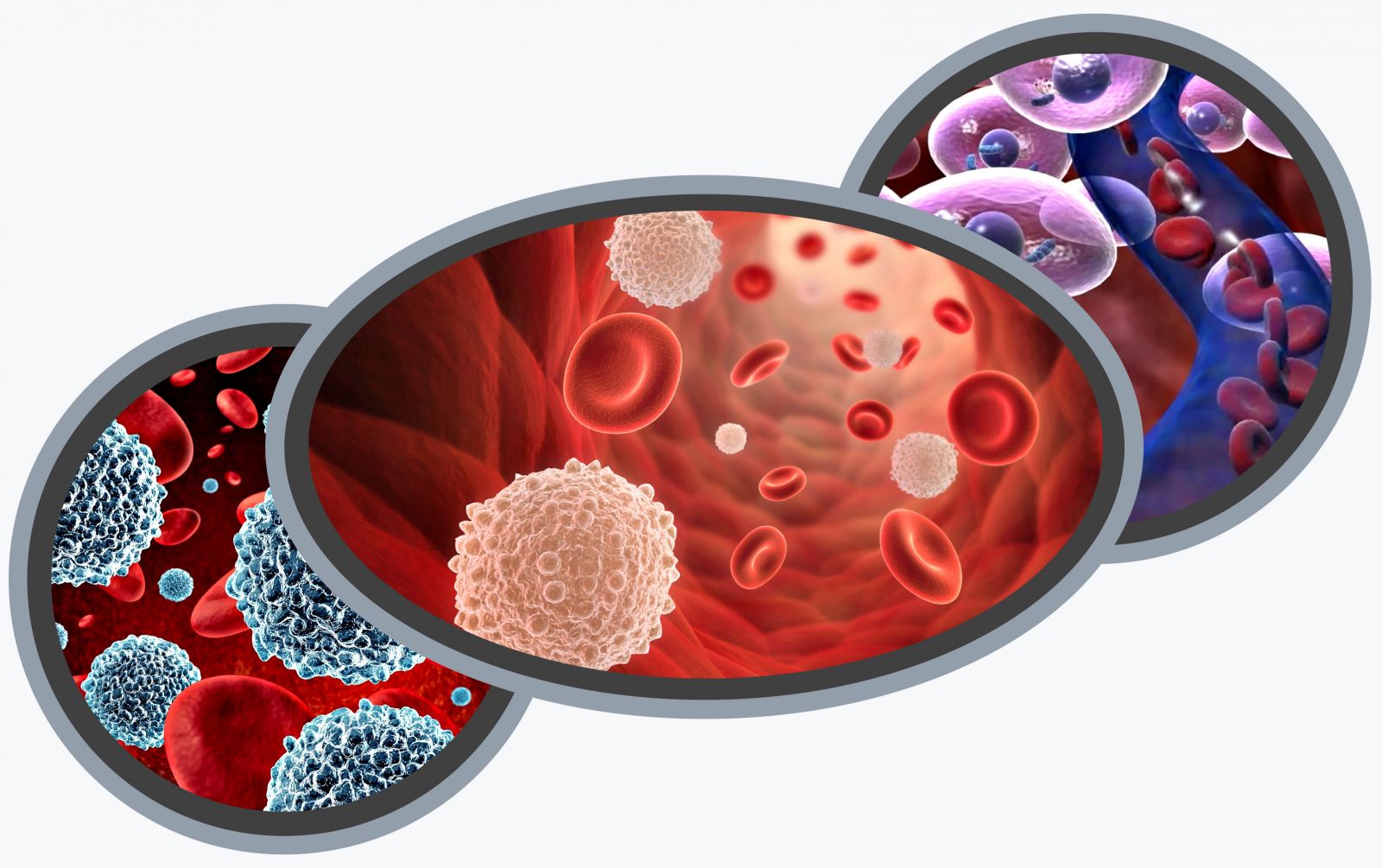
Outside the cell, nitric oxide signaling drives vasodilation which improves micro-circulation in the damaged tissue delivering oxygen, vital sugars, proteins and salts while removing waste. These mechanisms of action have been proved by over 40 years of laboratory experiments using lasers of minimal power. The recent development of higher-power class systems affords the clinician the ability to efficiently deliver adequate doses of light deep into tissue to reduce pain, inflammation, and accelerate healing.
