Scar tissue damage and fascia trauma have long been recognized in neural therapy as a source of chronic pain as a result of autonomic nervous system (ANS) upregulation (stress). They are now known to affect stress levels, and form fascia and deep adhesions which cause pain and lead to disease.
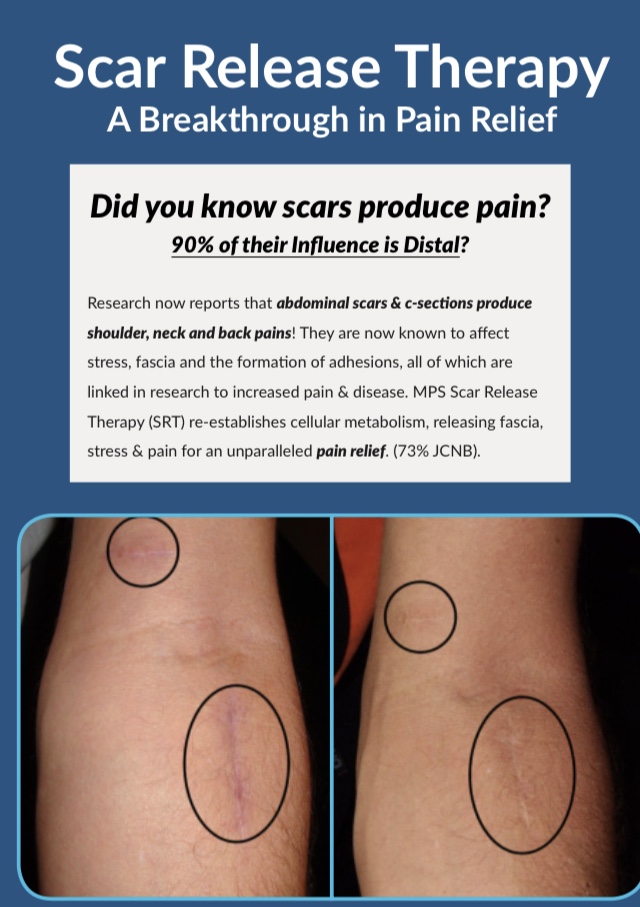
The application of MPS to the area of the scar and surrounding tissues re-establishes the metabolism in those areas that have been effectively cut off by the scar and releases the fascia to reduce stress and pain on surrounding tissues.
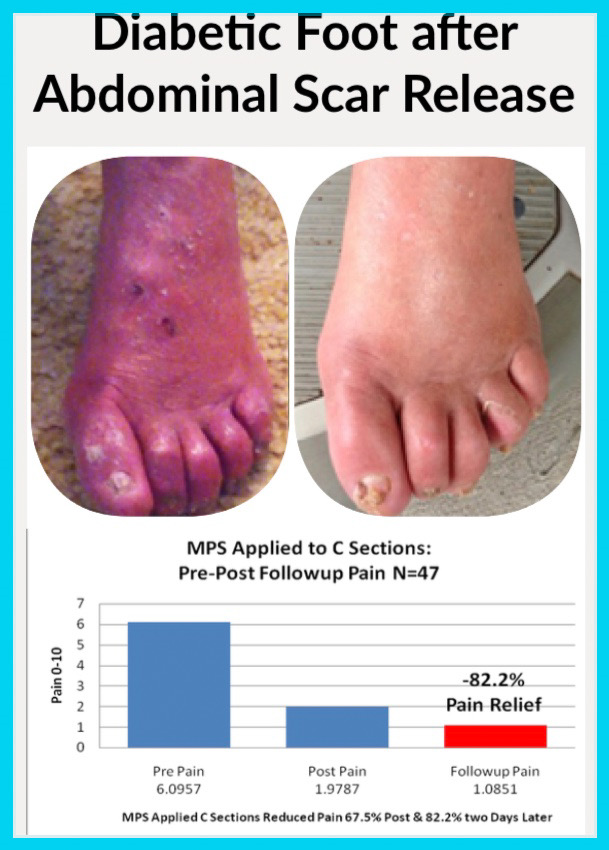
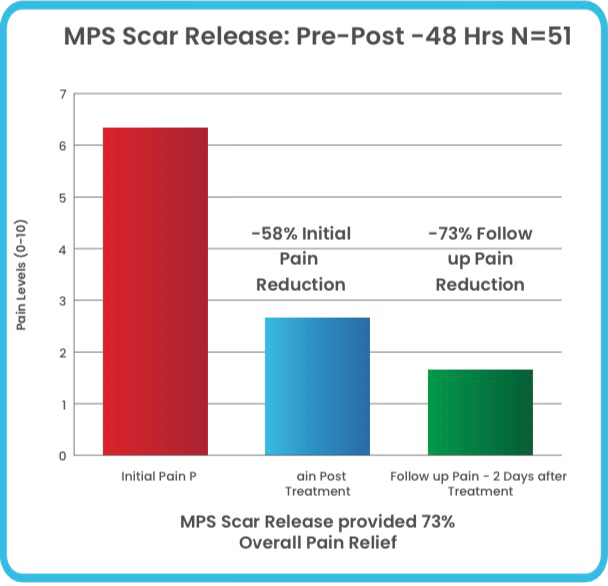
Type of Scars
Scar tissue presents in many different types, depending on the age of the person, skin type, skin condition, heredity and the severity of the wound
Some of the most common types are:
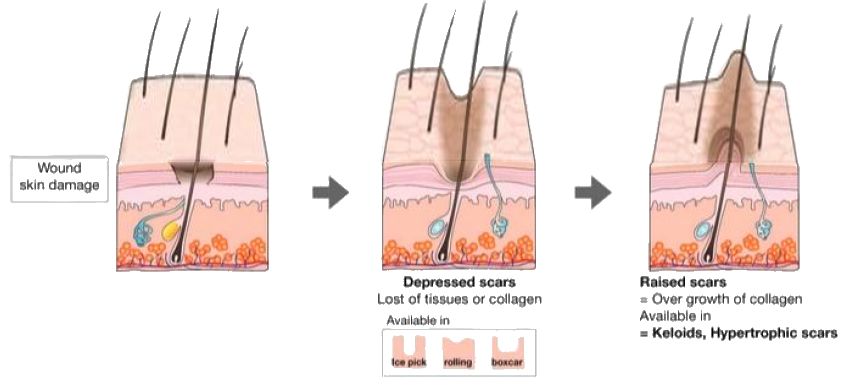
• Hypertrophic scars (raised and often red)
• Keloidal scars (much like hypertrophic, but spread far beyond the boundaries of the original injury)
• Atrophic scars (these leave depressions in the skin)
• Contracture scars (flat, tight scars that constrict movement, often caused by burns)
• Acne scars (pitting caused by the stretching of pores)
How MPS Scar/Adhesion Release Therapy works
In most cases scars will produce a tightening of the surrounding tissues that restrict either movement or function within the body. These restrictions can affect joints, limbs, muscles, organs, blood flow, lymphatic flow, and metabolic processes. Scar tissue has the potential to continue to grow and spread in any direction which is why it can affect so many areas of the body. MPS (Micro current Point Stimulation) can release the scar tissue and restore the flow of fluids, improve ROM (range of motion), reduce or remove complications caused by scaring and the pain associated with scars.
Scars form when there is an injury to the dermis, the deep, thick layer of skin. These scars form after the wound is completely healed. When scars form on an injury site the body responds in three stages. Inflammation is the first response which creates a blood clot to close the injury. The body then begins to make new cells to build a scab around the injury to prevent infections. When the injury is healed the body begins to remodel the area.
Stage 1: The Inflammatory Stage
The length of the inflammatory stage depends largely on the severity of the injury. It is defined by redness and swelling around the injury. It immediately goes to work creating a blood clot to stop the bleeding and antibodies are released to fight bacterial infections. A scab forms over the injury to protect the skin that is being regenerated. Increased blood flow in the area aids in new skin being steadily formed which causes discoloration.
Stage 2: Proliferative Stage
The length of this stage is 2-4 weeks, again depending on the severity of the injury. Fibroblasts, a type of biological cell that synthesizes the extracellular matrix and collagen, begin working around the entire injury. Fibroblasts produces the structural framework of our tissues and plays a critical role in healing. It begins with the scab to seal the wound to allow healing to proceed beneath it. It then begins to produce collagen, new skin tissue, that will emerge once the scab falls off. During this stage of new skin production new blood vessels are also formed to reconnect the broken tissues. This is the stage where the type of scar is determined. Depending on the metabolic rate of healing in the individual either just enough collagen formation will occur, or it will exceed what is needed.
Stage 3: Remodeling Stage
The remodeling stage begins after the injury is healed and the scab falls away. The body is still working on the injury both inside and outside. The duration can be a few weeks to years depending on the severity and cause of the injury. In healthy individuals the stage lasts only long enough to replace what is needed to protect the body. If the injury was light a small flat scar will appear but, in most cases, fades through the years as skin cells are replaced. If the injury is severe, the scar will be more pronounce and likely permanent.
If health is compromised or the individual’s metabolic rate of healing is highly active the production of collagen can continue for years increasing the size and depth of the scar. When this happens, the tissue surrounding the scar, as well as the scar itself, begins to tighten and can constrict the flow of blood, lymphatic and other fluids, decrease the range of motion, and cause discomfort. In severe cases it begins to constrict the flow of nutrients to the area and can affect muscle, nerve, and cell communication between the area and the brain, this leads to numbness in the area. As you can see scars can lead to serious conditions and illnesses depending on its location.
MPS
MPS is the method used to release scars and is especially effective in treating large, deep, painful scars. The term ‘release’ refers to the releasing or relaxing of contracted and tightened tissue.
MPS Scar/Adhesion Release Therapy (SRT) significantly reduces the restrictions of scar tissue. When used in combination with cold laser therapy the results are generally highly positive.
Using the micro current probes on the surrounding scar tissue results in several actions. First it stimulates a healing inflammatory response causing the body to react to the tissue as a foreign invader. The scar tissue is broken down and becomes dead cell waste. Circulation to the area is increased and the lymphatic system scoops up and excretes the dead cells from the body. The severity and how far it has spread beneath the skin surface will determine the length of treatment. The appearance of the scar will begin to visibly change and begin to reduce in size and depth. Scars from surgeries, gunshot injuries and even burns have shown amazing success with MPS.
Since the body’s fascial system is interconnected, a restriction or adhesion in one area will often affect other areas and result in compensation patterns and pain. When a scar has been released there is no longer a restriction in the flow of communication, blood circulation and lymph drainage. The body can then complete the healing process.
